Pain that travels from the back into the legs, numbness that appears while walking, or weakness that makes simple movements uncomfortable are often signs of nerve compression in the spine. Many people try medication, physiotherapy, or rest for months before realising the problem is not settling on its own.
When conservative treatment fails, spine decompression surgery becomes a well-established option to relieve pressure on affected nerves and restore mobility.
Under the care of Dr Purnajyoti Banerjee, patients receive careful assessment for spine decompression surgery in London, and evidence-based surgical planning focused on long-term relief. This ensures safe recovery and a confident return to daily activities.
What is spine decompression surgery?
Spine decompression surgery aims to relieve pressure on spinal nerves compressed by surrounding tissues. This pressure usually stems from bone overgrowth, bulging discs, or thickened ligaments.
It is designed to:
- Remove or reduce the element compressing the nerve
- Reduce pain, numbness or weakness
- Improve mobility and quality of life
Rather than just managing pain, the surgery treats the structural cause of symptoms.
Why does nerve compression cause pain and numbness?
Nerves are like electrical cables; when they’re compressed, signals don’t travel smoothly.
This miscommunication shows up as:
- Pain radiating down the arms or legs
- Tingling or numbness
- Weakness or “heaviness” in muscles
- Difficulty balancing or walking
Fixing the compression lets signals flow more normally again.
Who usually needs spine decompression surgery?
Surgery is not the first step for most patients. People typically try weeks of physiotherapy, medications, epidural injections, and lifestyle modifications first. Surgery becomes an option when:
- Pain doesn’t improve with non-surgical care
- Symptoms limit walking, work, or sleep
- Weakness or numbness increases
- MRI/CT confirms nerve compression
The decision is based on how symptoms affect daily life, not scans alone.
Why is lumbar decompression surgery commonly advised?
Lumbar decompression surgery focuses on the lower back, where nerve compression often causes leg pain and trouble walking rather than just back pain. With age-related changes or degenerative disc disease, the space around nerve roots narrows, leading to pain and mobility limitations.
According to UK clinical data, lumbar decompression surgery often leads to significant improvement in leg pain and walking capacity, helping many people return to activities they had stopped avoiding. (Source)
What happens during a laminectomy procedure?

During the operation:
- A small incision is made over the affected area
- The bone and tissue compressing the nerve are removed
- Nerves are protected throughout
- Stability of the spine is preserved wherever possible
The goal is simple: more room for the nerves, less pain for the patient.
How does a discectomy relieve nerve compression?
The discectomy/microdiscectomy procedure targets disc material that is pushing directly on nerve roots. Microdiscectomy uses magnification and very small instruments to reduce tissue disruption.
Research shows:
- Lumbar disc surgery (including microdiscectomy) yields good to excellent results in approximately 78–95% of patients at 1–2 years postoperatively. (Source)
- Microdiscectomy in clinical series often results in pain relief in the majority of people treated.
It’s one of the most commonly performed decompression techniques because of this consistency.
When are foraminotomy and laminotomy used?
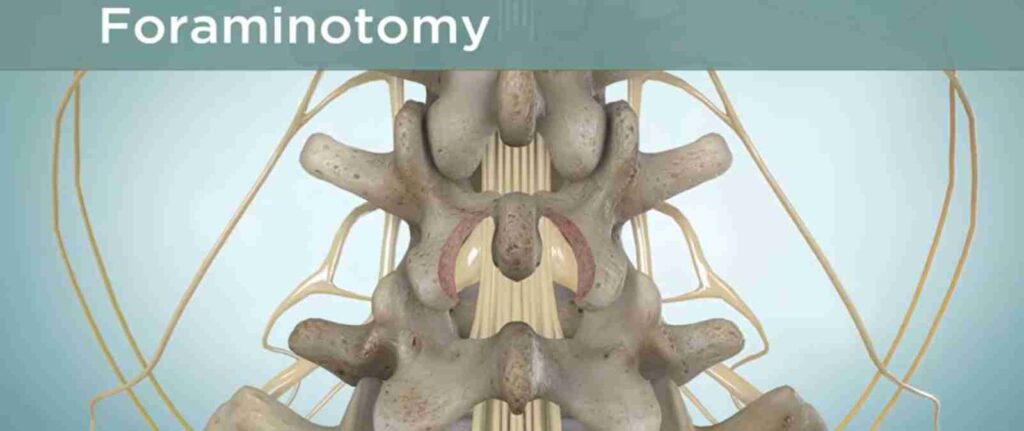
Foraminotomy/laminotomy are more focused decompression techniques targeting smaller nerve exit points rather than the entire canal. These are chosen when compression is localised, and a full laminectomy isn’t necessary.
Surgeons prefer these when the problem affects a single nerve root or when preservation of spinal structure is especially important.
How does spinal stenosis surgery improve walking ability?
Spinal stenosis surgery treats the narrowing of the spinal canal that compresses the nerves, particularly during walking or standing. This narrowing often causes leg pain that improves with forward bending or sitting.
In systematic reviews, lumbar decompression has been shown to significantly improve both leg pain and physical function in appropriately selected patients.
Is spine decompression the same as pinched nerve surgery?
Yes — patients often call it pinched nerve surgery in the spine (nerve compression intent). The medical goal is to release the structure compressing the nerve.
Compression may come from:
- Bone spurs
- Disc protrusions
- Thickened ligaments
Once the pressure is relieved, the nerve has a better chance to recover. Consult Dr Purnajyoti Banerjee, an expert in spine decompression surgery in London, who can offer expert guidance.
What happens immediately after spine decompression surgery?
Most patients start moving the same day or the next. Early mobility helps prevent stiffness and accelerates recovery.
Initial post-op care includes:
- Pain control
- Safe movement guidance
- Wound care
- Physiotherapy planning
Hospital stays for decompression procedures are usually short.
What should patients expect after a laminectomy?
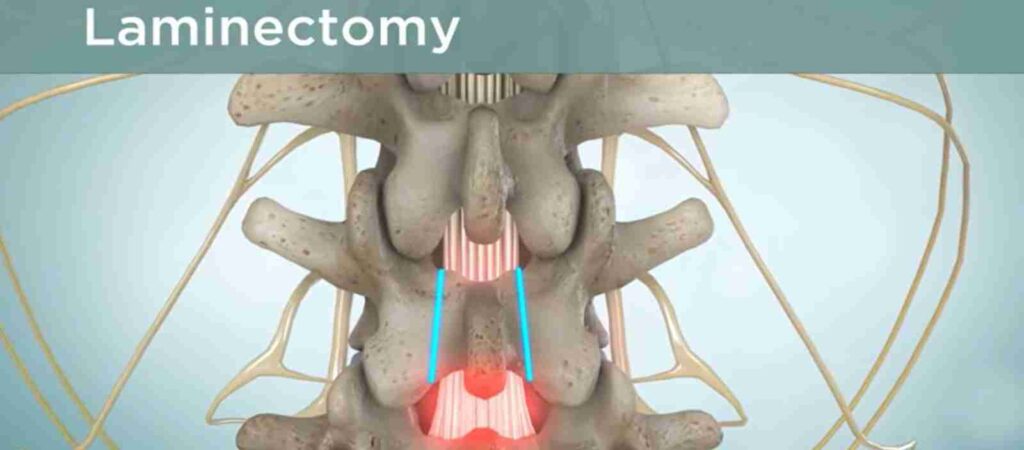
What to expect after a laminectomy varies with health status and the extent of the procedure. Some surgical soreness is normal, but nerve-specific pain often improves within days to weeks.
Patients typically notice:
- Reduced leg pain first
- Improved mobility
- Gradual return of strength
- Continued recovery over the months
This recovery pattern is supported by data indicating that improvements can occur soon after surgery.
How long does recovery take after lumbar decompression surgery?
Recovery is not instantaneous, but it is predictable with effective rehabilitation.
Typical milestones include:
- Walking within 24 hours
- Light activities within 2–3 weeks
- Structured physiotherapy for 4–6 weeks
- Functional recovery within 3–6 months
Consistency in rehabilitation makes a real difference.
How successful is spine decompression surgery?
While any surgery has nuances, decompression tends to deliver meaningful improvement for most patients.
Clinical outcome studies show:
- Lumbar disc decompression procedures generally yield 80–90% good-to-excellent outcomes. (Source)
- Many patients experience a significant reduction in pain and improved walking ability compared with pre-surgery status.
Success depends on proper patient selection and realistic expectations.
Confidence Comes from Clarity
Spine decompression surgery is not about dramatic cuts or drastic reconstruction. It’s about targeted relief of nerve pressure that has been disrupting normal life.
When conservative care stops working and nerves are clearly compromised, decompression can reduce pain, improve function, and restore quality of life. Understanding what occurs in the operating room and how recovery unfolds transforms uncertainty into informed choice.
Get personalised care for spinal decompression surgery in London. Email Dr Purnajyoti Banerjee: purnajyoti74@gmail.com
People Also Ask
1. What is spine decompression surgery used for?
Spine decompression surgery is used to relieve pressure on spinal nerves caused by disc bulges, bone overgrowth, or spinal narrowing. It helps reduce pain, numbness, and weakness linked to nerve compression.
2. How do I know if I need spine decompression surgery?
You may need spine decompression surgery if pain, numbness, or weakness persists despite physiotherapy and medication. Imaging tests like MRI usually confirm nerve compression before surgery is advised.
3. Is spine decompression surgery a major surgery?
Spine decompression surgery is considered a standard surgical procedure, but many techniques are minimally invasive. Recovery is often faster than that of traditional open spine surgeries.
4. What conditions are treated with spine decompression surgery?
It is commonly used to treat disc herniation, spinal stenosis, nerve compression, and degenerative spine conditions. These problems cause pressure on nerves, leading to pain and mobility issues.
5. How long does spine decompression surgery take?
Most spine decompression surgeries take between one and two hours, depending on the procedure and the number of levels treated. Your surgeon will confirm the expected duration beforehand.
6. Is spine decompression surgery painful?
Some post-surgical discomfort is normal, but nerve-related pain usually improves early. Pain is managed with medication and gradually reduces as healing progresses.
7. How successful is spine decompression surgery?
Studies indicate that approximately 70–90% of appropriately selected patients experience significant symptom improvement. Success depends on accurate diagnosis, timing, and post-operative rehabilitation.
8. What is the recovery time after spine decompression surgery?
Most patients are ambulating within 24 hours and resume light activities within a few weeks. Full recovery typically takes three to six months with proper rehabilitation.
9. Are there risks or complications with spine decompression surgery?
As with any surgery, risks include infection, bleeding, and nerve irritation; however, serious complications are uncommon. Careful surgical technique significantly reduces these risks.
10. When should I see a spine surgeon for nerve compression?
You should consult a spine surgeon if pain, numbness, or weakness persists for several weeks despite treatment. Early evaluation helps prevent long-term nerve damage.